In brief:
- The pilonidal cyst is a benign condition, more common in men but can affect women, especially young women between 15 and 40 years old.
- It forms due to irritation from one or more ingrown hairs in the intergluteal cleft, triggering an inflammatory reaction.
- Symptoms include a hard nodule, painful if infected, sometimes accompanied by suppuration and abscesses.
- Several causes favor its appearance: hairiness, depth of the intergluteal fold, smoking, overweight, prolonged sitting position…
- Treatment mainly relies on surgery or laser intervention, with long postoperative care necessary to avoid recurrence and complications.
- Proper management and prevention focused on hygiene and body habits help limit risks.
The origins of the pilonidal cyst in women: understanding formation and underlying causes
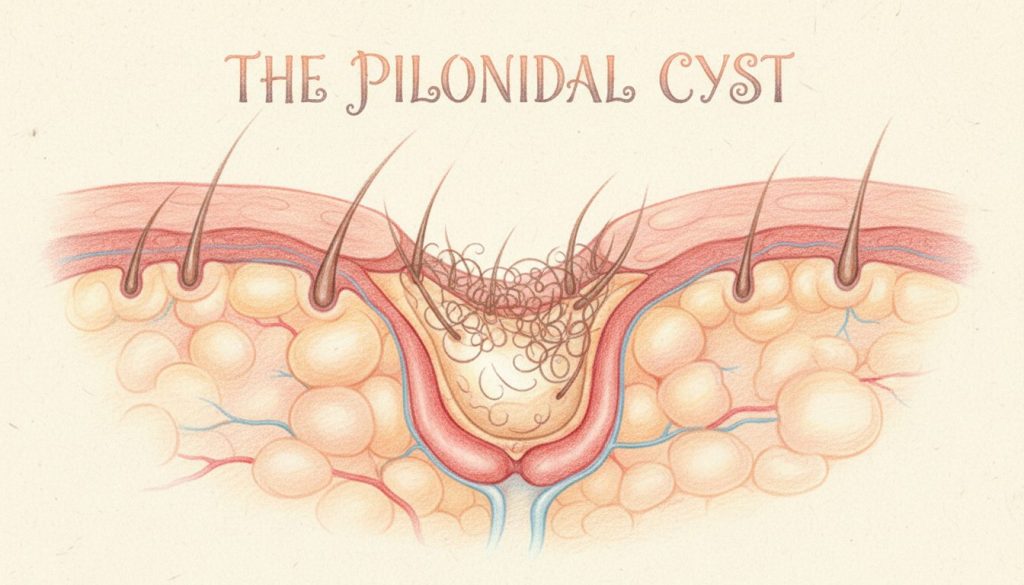
The pilonidal cyst, sometimes called sacrococcygeal cyst, corresponds to a benign pathology affecting the skin at the level of the intergluteal cleft, the area located between the two buttocks. While this condition is generally more recorded in men, it does not spare women, particularly young adults aged between 15 and 40 years.
The genesis of the pilonidal cyst is based on prolonged irritation caused by hairs that penetrate the epidermis, thus bursting as foreign bodies for the organism. According to dermatologist Erwin Benassaia, these ingrown hairs stimulate an intense inflammatory reaction, accompanied by an accumulation of sebum and cellular debris contributing to the painful formation of the cyst.
Two main origins are distinguished: the cyst can be congenital, present from birth as an anomaly of the intergluteal cleft, or acquired, meaning resulting from the penetration of an ingrown hair. In women, some factors related to their anatomy and lifestyle can favor this pathology, especially:
- The depth and narrowness of the intergluteal fold that traps hairs more easily.
- Dense or thick hairiness, which increases the risk that hairs become cystic.
- Insufficient or poorly adapted hygiene, leading to greasy skin rich in sebum, a favorable environment for inflammation.
- Smoking, which alters skin defenses and slows healing.
- Overweight, providing a setting conducive to intense friction and microtraumas.
- Prolonged seated positions, often encountered professionally, which can increase pressure in this area.
- Repeated friction from tight clothing or targeted physical activities.
Sometimes added to these factors is a more fragile hormonal or immunological context, which can exacerbate the local inflammatory reaction. The intersection of these causes highlights the complexity of this formation, which is not reduced to a simple superficial problem but reflects a subtle interaction between the skin environment, lifestyle, and individual predispositions.
Insights into the involved biological mechanisms
The skin in the intergluteal area is constantly exposed to humidity, high temperature, and chronic friction. These conditions promote rupture of hair follicles and the formation of sinuous pathways in the dermal depth where curled or broken hairs settle, difficult to expel naturally. The body then reacts by forming a cystic capsule to “trap” this foreign body, generating inflammation and pain.
This mechanism explains why recurrences are frequent and why simply evacuating the cyst is insufficient without treating the terrain conducive to its formation. Thus, the therapeutic approach must include advice to limit excessive hairiness, improve skin quality, and moderate aggravating factors.
Recognizing the symptoms of pilonidal cyst in women: visible signs and evocative pains
Detecting a pilonidal cyst in women relies on careful observation and body listening for unusual sensations. In its initial form, this nodule manifests as a small firm lump, implanted in the intergluteal cleft, sometimes imperceptible without careful palpation.
When superinfection occurs, the pain becomes sharper and persistent, described as pulsatile. This pain is often aggravated by sitting posture, prolonged walking, or certain sports involving the region. On clinical examination, the area may appear red, swollen, and warm to the touch, a sign of localized abscess. Sometimes, purulent discharge or small fistulas may externalize at the cyst opening.
Symptoms can thus extend over several days to weeks if treatment is delayed, increasing the risk of complications, notably the spread of infection to adjacent tissues.
Differentiating the pilonidal cyst from other similar conditions
It is essential to distinguish the pilonidal cyst from other localized pains or masses, such as anal abscesses, boils, or hemorrhoids. Clinical context, combined with examination by a healthcare professional, allows diagnosis based on typical localization and characteristic appearance of the cyst.
Biopsy or medical imaging are rarely necessary except in suspected extensive involvement or doubtful diagnosis.
- Main symptoms: local pain, abnormal sensitivity, red swelling.
- Secondary manifestations: purulent discharge, persistent inflammation, functional discomfort.
The symptomatic profile then guides appropriate treatment, considering the severity and duration of the inflammatory lesion.
Treatment options for pilonidal cyst in women: surgery, laser, and alternatives
Faced with a pilonidal cyst, the therapeutic approach is crucial to prevent chronicity or the formation of a painful abscess. Treatment should ideally be undertaken outside acute inflammation episodes to limit complications.
Two main techniques are considered effective:
- Classic surgery: performed under general anesthesia on an outpatient basis, this intervention involves completely removing the cyst. Postoperative period can be long, with an open wound left to avoid any recurrence. This healing window generally lasts about two months, requiring regular care and rest.
- Laser treatment: this less invasive approach is performed under local anesthesia. Faster and often better tolerated, it allows targeted evacuation of the cyst but carries a higher risk of recurrence, necessitating close follow-up.
Beyond these interventions, non-surgical measures can strengthen prevention of new lesions or minimize aggravating factors:
- Rigorous daily hygiene monitoring, using mild soaps and thorough drying.
- Reduction of local hairiness by appropriate and non-aggressive methods.
- Modification of lifestyle habits such as limiting continuous sitting time and choosing natural fiber clothing.
- Smoking cessation, essential to optimize healing and reduce infection risk.
| Treatment | Advantages | Disadvantages | Duration of postoperative care |
|---|---|---|---|
| Classic surgery | Complete eradication, low recurrence rate | Long care, open wound, temporary functional discomfort | About 2 months |
| Laser | Less invasive, local anesthesia, quick recovery | Increased risk of recurrence | Several weeks |
It is important to remember that self-treatment is discouraged for a pilonidal cyst, to avoid any worsening or complications. Medical consultation is imperative for a personalized assessment and appropriate management.
Living with a pilonidal cyst: managing pain, preventing infection, and improving daily comfort
Although benign, a pilonidal cyst can significantly impact well-being, especially when it becomes painful or infected. Understanding how to live with it and adopting protective reflexes are fundamental aspects of care and relief.
Pain, often described as sharp and pulsatile during inflammatory flare-ups, sometimes limits activities, especially those involving prolonged sitting or repetitive movements. To relieve this discomfort:
- Use appropriate cushions to lighten pressure on the intergluteal cleft.
- Use prescribed anti-inflammatory drugs and strictly follow medical recommendations.
- Take lukewarm showers promoting muscle relaxation rather than prolonged baths.
Infection is the main trigger of complications: an abscess may form, increasing pain and making surgical treatment urgent. Careful daily hygiene combined with constant vigilance on symptom evolution ensures effective monitoring.
Moreover, emotional management of this pathology remains crucial, as it affects an intimate area prone to discomfort and modesty. Caring support helps restore confidence in one’s body and in the ability to heal without stigmatization.
Practical advice to improve quality of life
- Avoid tight or synthetic clothing that promotes sweating and friction.
- Practice gentle physical activity limiting prolonged immobility while improving local blood circulation.
- Maintain a balanced diet to preserve a healthy weight and an active immune system.
Prevention of the pilonidal cyst in women: strategies to reduce risks
Prevention is an essential component to avoid the appearance or recurrence of the pilonidal cyst. In this context, several measures can be implemented, combined with thorough knowledge of causes and risk factors:
Firstly, attention to local hairiness plays a primary role. Regular but gentle hair removal, adapted to skin sensitivity, limits ingrown hair formation. The use of mild exfoliants made from natural ingredients can help prevent follicle obstruction.
Then, managing comfort in daily life is fundamental: avoid prolonged sitting, prioritize active breaks, and choose comfortable seats adapted to morphology.
Improving body hygiene is imperative with non-aggressive products and meticulous drying of the intergluteal area, often overlooked but sensitive to humidity and bacteria. Wearing underwear made of soft natural fibers also provides an additional protective barrier.
Finally, quitting smoking represents a decisive lever in preventing infections and improving healing quality, as regularly emphasized by the medical community. Similarly, maintaining a balanced weight helps limit pressure and friction in this exposed area.
Simple habits to integrate daily
- Practice adapted and regular hair removal.
- Take care of the skin with mild and natural cleansers.
- Favor moderate and regular physical activity.
- Take frequent breaks when sitting for long periods.
- Arm yourself with patience and kindness in skin care management.
Is the pilonidal cyst contagious?
No, the pilonidal cyst is not contagious. It results from local irritation related to ingrown hairs and an inflammatory reaction.
Can a pilonidal cyst be prevented only with good hygiene?
Although good hygiene is essential, it is not always sufficient to prevent a pilonidal cyst. Other factors such as hairiness, area morphology, or prolonged sitting also play a role.
Is pilonidal cyst surgery painful?
Surgery is performed under general or local anesthesia, so it is painless during the operation. However, postoperative care may cause temporary local pain managed with appropriate treatment.
Is laser a definitive solution for treating pilonidal cyst?
Laser can be a less invasive alternative, but there is a higher risk of recurrence. The choice of method depends on personalized medical evaluation.
What are the signs of an infection of the pilonidal cyst?
Intense pain, redness, warm and sensitive swelling, sometimes purulent discharge are signs that require prompt consultation.