In brief
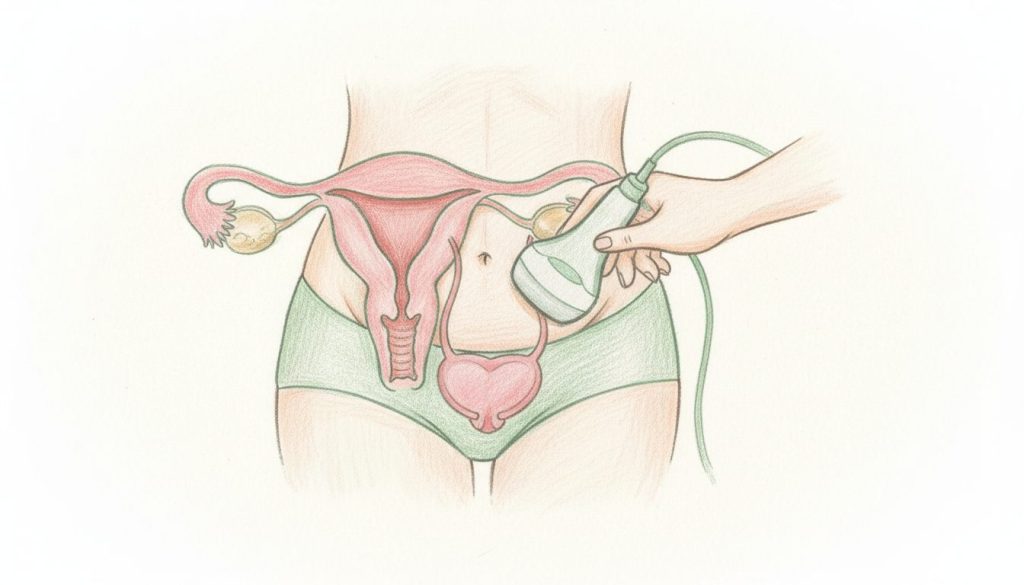
- Pelvic ultrasound offers a non-invasive visualization of essential pelvic organs such as the uterus, ovaries, and bladder.
- There are two main modalities: abdominal ultrasound, external and quick, and endovaginal ultrasound, more precise due to the proximity of the organs.
- Each procedure is tailored to a specific indication, ranging from gynecological follow-up to pregnancy monitoring, and even fertility.
- Preparation generally remains simple, with a few precautions to optimize images and ensure comfort.
- Advances in medical imaging technology now enable extremely precise pelvic diagnoses, aiding care management in gynecology.
How pelvic ultrasound works: principles and physical principles of medical imaging
Pelvic ultrasound relies on a medical imaging technology using sonography, that is high-frequency ultrasounds. Like bats or dolphins, the devices emit sound waves that pass through tissues and bounce back depending on their density and composition. A device, usually a probe, captures these reflected echoes and translates them into images visible on a screen.
Constantly redesigned, this technology involves no ionizing radiation source, thus protecting the patient from side effects linked to conventional X-rays. Since these waves are inaudible, the exam proceeds without sound discomfort.
The value of pelvic ultrasound lies in its ability to observe in real time the pelvic anatomy: the bladder, uterus, cervix, ovaries, and fallopian tubes. This visualization reveals details essential to a precise pelvic diagnosis, notably in gynecology.
Moreover, the smoothness of the exam allows capturing physiological movements, for example blood flow thanks to the Doppler effect. This improvement broadens the scope of analysis to organ vascularization, important in certain pathologies.
The variety of techniques between abdominal and endovaginal ultrasound thus stems from the effort to optimize image quality depending on the clinical situation. The abdominal probe, minimally intrusive, glides over the skin of the lower abdomen, whereas the endovaginal probe, more discreet, is inserted into the vagina to get closer to the organs and appreciate subtler details. Adjusting technical parameters remains a matter of expertise, where the sonographer’s skill often makes the difference.

Reasons for a pelvic ultrasound exam: clinical indications and benefits in gynecology
Pelvic ultrasound, abdominal or endovaginal, is only performed with a medical prescription, within a specific framework. It is used in several clinical contexts, each requiring a delicate and adapted approach.
Investigation of unusual gynecological symptoms
The occurrence of pelvic pain, unexpected bleeding, or menstrual cycle disorders often prompts ultrasound investigation. This procedure seeks pathologies such as uterine fibroids, ovarian cysts, or signs of endometriosis. By observing the morphology and texture of the organs, ultrasound sharpens the clinician’s understanding of these symptoms.
Pregnancy follow-up and fetal development monitoring
During prenatal follow-up, pelvic ultrasound takes on critical importance. Beyond simply confirming pregnancy, it assesses embryo location, progress, and heartbeat. The method chosen for the exam depends on the stage of pregnancy. In the first trimester, endovaginal ultrasound provides better resolution, essential to examine every detail of embryonic development.
Assistance in medically assisted procreation
Within the planning and monitoring of in vitro fertilization (IVF) or other assisted reproductive techniques (ART), ultrasound precision is paramount. It estimates the number and size of ovarian follicles, a key parameter for successful ovarian stimulation.
Screening and monitoring of gynecological abnormalities
Finally, pelvic ultrasound accompanies screening assessments. Whether for routine control or cancer surveillance, this exam facilitates non-invasive, respectful, and reassuring observation, a key element in ongoing medical follow-up.
Coherence in indications combined with the trust established between patient and practitioner influences the overall experience, often calming anxieties linked to this imaging.
Preparation and procedure for abdominal and endovaginal pelvic ultrasound
Preparing for a pelvic ultrasound procedure generally does not require significant effort. That said, some precautions facilitate obtaining optimal results while maintaining personal comfort.
Specific preparation depending on the type of ultrasound
For abdominal ultrasound, it is often recommended to arrive with a full bladder. This distension improves the visibility of pelvic organs by moving the intestines out of the field of view. However, with advances in devices in 2026, this constraint is sometimes relaxed, except for targeted exams such as endometriosis screening.
In contrast, endovaginal ultrasound does not require a full bladder, offering increased comfort. It is recommended to avoid applying creams or oils on the pelvic area before the exam, as they could hinder ultrasound transmission.
Step-by-step procedure
After a kind and explanatory exchange, the patient lies down comfortably, knees slightly bent. For abdominal ultrasound, the probe is coated with aquatic gel and gently slid over the lower abdomen surface. For endovaginal ultrasound, a thin probe, protected by a latex or silicone sheath, is inserted into the vagina, sometimes with the patient’s help if she wishes.
The practitioner then slowly directs the probe to sweep the targeted areas, observing in real-time on a dedicated screen. This dynamic visualization allows taking precise measurements, evaluating tissue texture, and detecting any abnormality.
The total duration of the exam often varies between 15 and 30 minutes. Each step seeks to be respectful, leaving room for questions and answers to dispel any apprehension.
The level of discomfort varies from person to person. Endovaginal ultrasound may cause a sensation of discomfort but should never be painful. At the slightest pain, it is recommended to report it immediately to adapt the manipulation.
Comparative table of the two pelvic ultrasound techniques
| Criterion | Abdominal ultrasound | Endovaginal ultrasound |
|---|---|---|
| Technique | Probe applied on the lower abdomen | Probe inserted into the vagina |
| Precision | Good, but limited by distance | Very high, allows better resolution |
| Comfort | Non-invasive, generally comfortable | May be slightly uncomfortable, but without pain |
| Preparation | Often full bladder | No need for a full bladder |
| Applications | Routine exam, advanced pregnancies | Early pregnancy, ART, detailed exploration |
Feelings and precautions for a calm exam: between gentleness and kindness
When it comes to the intimate sphere, feelings of apprehension are often present. This is an additional reason to choose a caring practitioner, capable of establishing a climate of trust, essential to the success of a precise and respectful ultrasound procedure.
The freedom to accept or refuse endovaginal ultrasound is a fundamental principle. No patient should ever feel forced. Some women, especially those who have not had sexual intercourse with penetration, may prefer to opt for abdominal ultrasound, which is completely external and painless.
In case of pain or discomfort, open communication with the healthcare professional is essential. Any technique adjustment is possible to ensure a gentler passage. This freedom of expression during the exam helps ease tensions, fostering a moment where gentleness and efficiency intertwine.
From a hygienic point of view, the probe covers are single-use and sterile. They ensure maximum safety, essential in the context of excellent medical imaging.
One last point concerns latex allergies: it is essential to report this beforehand so that suitable covers are used to preserve skin integrity and the serenity of the exam.
Costs, reimbursements, and access to pelvic ultrasound: an accessible and regulated process
In 2026, pelvic ultrasound remains an accessible exam in most specialized offices, whether with the gynecologist, the sonographer midwife, or the radiologist. The price generally ranges between 52 and 70 euros, reflecting the technical and human quality provided at each consultation.
Coverage by Social Security is generally about 70%, thus covering most of the costs related to this essential gynecological exam. Health insurance complements, present in most current contracts, usually cover the rest, notably in case of extra fees.
The democratization of skills, notably with the integration of sonographer midwives in the medical landscape for several years, helps reduce waiting times and offer more personalized support.
Finally, personal investment in undergoing a pelvic ultrasound is also a holistic care approach, where body and emotion meet. This underlines how this exam participates in a path of knowledge and soothing, fundamental in the parent-child relationship and future well-being.
What is the main difference between abdominal and endovaginal ultrasound?
Abdominal ultrasound uses an external probe placed on the belly, while endovaginal ultrasound uses a probe inserted into the vagina, offering more precise resolution. The choice between the two mainly depends on the analysis needs and patient comfort.
Is pelvic ultrasound painful?
The exam is not painful, but endovaginal ultrasound may cause slight discomfort. Any pain must be reported to adapt the procedure.
Should one come to the ultrasound with a full bladder?
It depends on the type of ultrasound and the indication. Abdominal ultrasound often requires a full bladder for better visibility, whereas endovaginal ultrasound does not. It is important to follow the practitioner’s instructions.
What are the main objectives of a pelvic ultrasound?
It allows visualization of pelvic organs such as the uterus, ovaries, and bladder to diagnose pathologies, monitor pregnancy, or assist in ART with precision.
Is pelvic ultrasound financially accessible?
Most exams cost between 52 and 70 euros, reimbursed at 70% by Social Security. Health insurance generally covers the remainder, making this exam accessible to a wide audience.